WALANT Technique Improves Patient Outcomes and Experience
WALANT Technique Improves Patient Outcomes and Experience
May 29, 2018
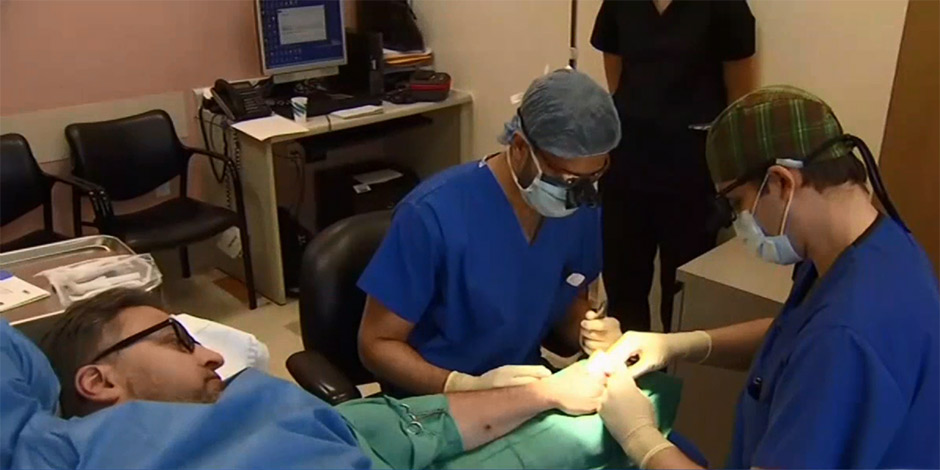
Steven M. Koehler, MD, director of Orthopedic Hand Surgery at NYC Health + Hospitals/Kings County, has become one of the first doctors in New York City, and likely the first in Brooklyn, to use an innovative method of hand surgery that allows patients to be awake during the outpatient procedure. Known as WALANT (an acronym for Wide Awake Local Anesthesia No Tourniquet), the surgical technique was first performed at NYC Health + Hospitals/Kings County on November 3, 2017—one of the first in New York City. It is believed that NYC Health + Hospitals/Kings County has the first and only ambulatory facility dedicated to wide-awake hand surgery—with no pre-operative testing or post-operative recovery or monitoring—in the city.
While traditional hand surgeries require general anesthesia and a tourniquet to stem the flow of blood through a vein or artery, the new technique requires neither. At NYC Health + Hospitals/Kings County, Dr. Koehler performs WALANT surgery in the hospital’s Ambulatory Care Clinic on patients who are awake during the entire process, which lasts approximately 45 minutes from check-in to check-out. Patients receive an anesthetic injected at the surgical site, epinephrine to stop bleeding, and lidocaine to subdue pain—the same medications commonly used in simple dental procedures.
The most common conditions for which WALANT surgery is available at NYC Health + Hospitals/Kings County include carpal tunnel release, follow-up surgeries after amputation (often called revision surgery), the removal of cysts that develop on the wrist (dorsal wrist ganglion excision), tendon repairs and transfers, reconstructive repair of wounds, and the removal of dead tissue or foreign objects.
“When patients are not sedated during surgery, they are able to receive education and more readily participate in their care,” said Dr. Koehler. “With the lack of sedation, their memory is not impaired, and they can leave right after the surgery, without having to recover from sedation or unnecessary opiates. They can ask questions and see a repair—perhaps a return of function—during the surgery. Educating the patient during surgery not only provides better outcomes and fewer complications, but is beneficial to the overall patient experience.”
Patients also benefit in other ways from WALANT surgery. They don’t need pre-operative procedures, such as EKGs or chest X-rays, nor do they need an anesthesia consultation. There’s no fasting or changing medication schedules beforehand, which is particularly important to those with diabetes. The procedure is quicker, and because the surgeon can perform more surgeries each day, there is typically less time to wait for an appointment than for traditional hand surgery. Importantly, there are also fewer complications.
In some cases, WALANT offers a treatment when traditional surgery is not an option. A recent example is a woman who needed repairs for cut tendons and nerves in her hand, but open surgery was contraindicated because she is pregnant.
“Everyone in health care is looking for ways to provide better care, and WALANT makes that possible,” said Dr. Koehler. “Plus, it frees up the operating room, the anesthesiologist, and the rest of the surgical team for procedures that really do need them.” One study found that carpal tunnel decompression, one potentially popular application of WALANT surgery, is nearly four times cheaper and twice as efficient when performed in an ambulatory setting using WALANT than in a traditional surgery setting.
“We are always looking for ways to improve patient care,” said Sheldon P. McLeod, chief executive officer at NYC Health + Hospitals/Kings County. “The WALANT technique for hand surgery is advantageous, because it reduces the need for sedation, and pain medication. This groundbreaking procedure allows us to provide advanced quality care for our patients.”
The WALANT surgical technique was developed largely in Canada, led by Canadian hand surgeon Dr. Don Lalonde. He has noted that the main challenge to pure local anesthesia and getting rid of the tourniquet was the myth that epinephrine injection in the finger commonly led to necrosis. In recent years, the procedure has become increasingly popular in Canada, as well as in England, China, and Brazil, among other countries. The nascent popularity in the United States is possible because no FDA approval was needed, since it is neither a device nor a new drug, and the drugs that are used have been used safely for decades.